We are a leading Healthcare and Life Sciences company with over 50 years of experience in the pursuit of health and well-being at our core.

Heritage
Our heritage gives us strength and capability to help enable healthy and happy communities.

Global Reach
Operations in over 23 countries across South East Asia, South Asia, Commonwealth of Independent States, Middle East and Africa.

Vast Range
We offer a vast range of over 200 products in major therapeutic categories.


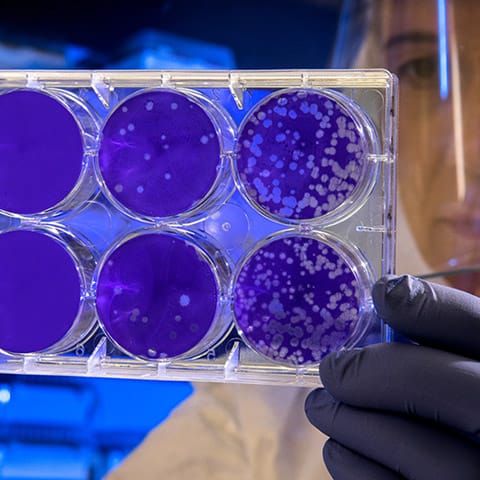
Our Commitment to Create Healthy Happy Lives
0+
Years in Business
0+
Countries
0+
Products
0+
Employees












